Improving EMR adoption and data quality across rural health posts in Rwanda
Executive summary
SFH Rwanda deployed an Electronic Medical Record (EMR) across rural health posts to gain real-time visibility into disease burden. Post-deployment, EMR usage and data quality fell short of expectations due to high clinician workload, duplicated data entry, and usability issues.
Through on-the-ground user research with nurses and digital health officers, I identified key friction points and led the UX research for two parallel interventions: simplifying the patient visit experience and enabling SFH to track EMR data quality at a facility level.
The work resulted in a redesigned patient visit flow that tested significantly easier to use, strong user preference for the new interface, and a data-quality tracking dashboard that allowed SFH to proactively support health posts. Together, these efforts contributed to improved completeness and consistency of EMR data while reducing clinician burden.
Reduction in task difficulty
Efficiency regression
User preference
Context
Client: Society for Family Health (SFH) Rwanda, Role: Product designer (UX research only), Timeline: January 2024 – April 2025
Health posts are the primary point of care in Rwanda’s rural health system. While an Electronic Medical Record (EMR) was deployed to capture patient-level clinical data, the realities of day-to-day work at health posts—high workload, duplicated reporting, and limited infrastructure—made consistent EMR use difficult. As a result, data quality suffered, limiting the usefulness of the EMR for understanding disease burden and planning interventions.
Problem
As part of an effort to digitise health care facilities and gain real-time visibility into disease burden at health posts, SFH partnered with eFiche to deploy an Electronic Medical Record (EMR).
Following deployment, it became clear that the EMR was not being used as effectively as expected. Basic analysis of EMR data revealed:
- Lower-than-expected patient visits captured
- Incomplete patient records
- Inaccurate or missing diagnoses
These issues limited the reliability of the data and reduced the value of the EMR for both SFH and the broader health system.
Research and Process
Because health posts operate in rural contexts, on-the-ground research was essential. I visited several health posts and conducted in-person interviews with nurses and digital health officers who used the EMR daily.
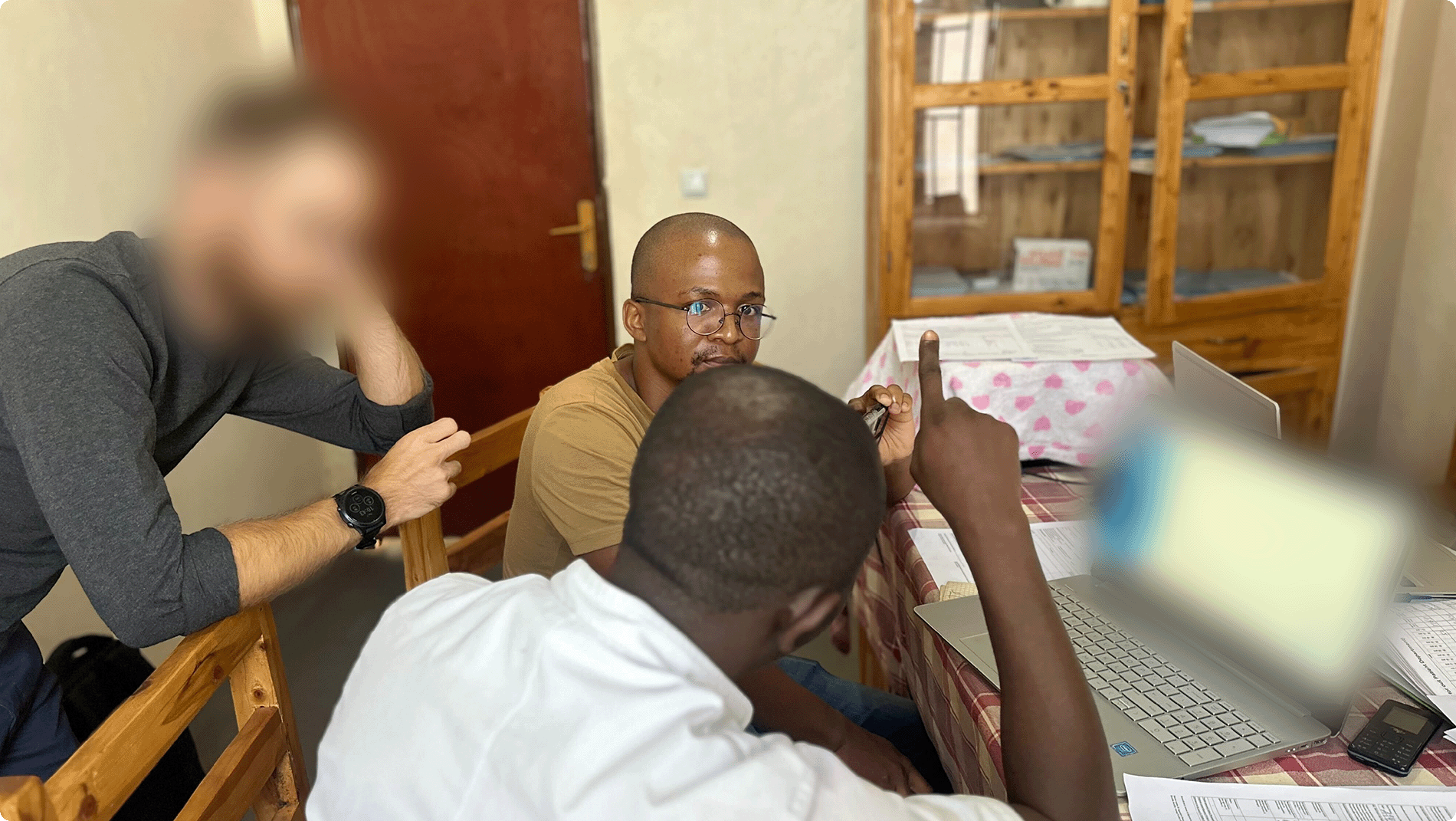
A key insight was the duplication of effort users faced. In addition to the EMR, they were required to complete the Ministry of Health’s paper patient register and the Rwanda Social Security Board’s (RSSB) insurance claims system. All three systems required largely the same information, and users felt much of this could be automated or simplified.
We also learned that the register and insurance systems could not be removed, and their data was inaccessible due to regulatory constraints. This meant any solution needed to work around these systems rather than replace them.
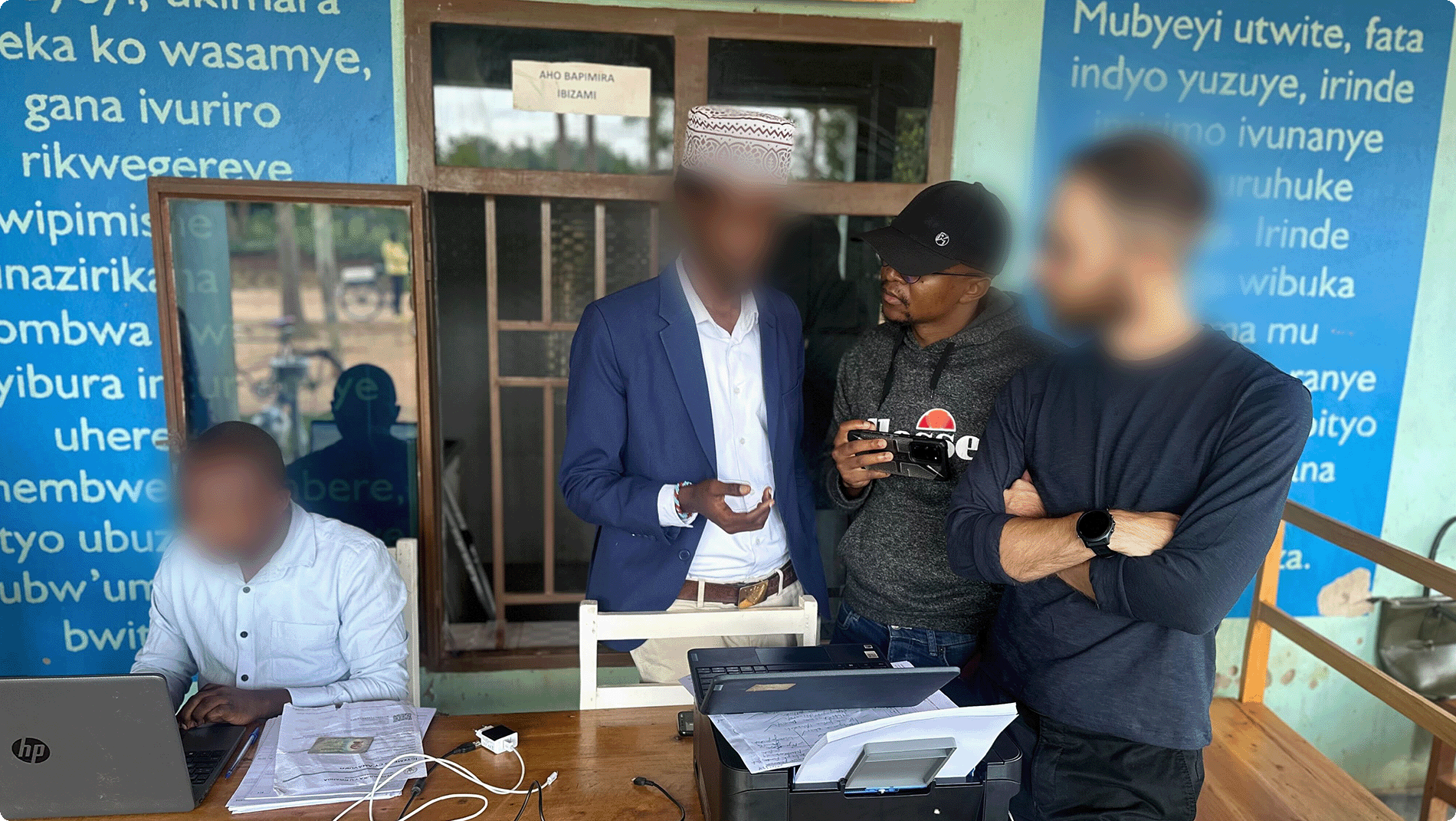
To validate and broaden these findings, we created a survey that collected feedback from all SFH-supported health posts. Analysis of the responses revealed relatively simple opportunities to reduce user burden.
In parallel, I conducted a heuristic evaluation of the EMR’s current state and identified usability issues such as:
- No notifications when lab results were ready
- Different patient forms depending on entry point
- Unclear role changes (e.g. nurse → doctor) when navigating between dashboards
Solution
Based on the interviews and survey results, we focused on two interim solutions: improving the patient visit experience and enabling SFH to track EMR data quality at a health-post level.
Improving the EMR
During a patient visit, clinicians had to complete six separate pages: Physical Examination, Diagnosis, Laboratory, Procedures, Patient Movement, and Prescriptions. These pages could be accessed in any order and required manual navigation, which often led to missing or incomplete information.
We identified an opportunity to combine these steps into a single, structured page that was easier to navigate and reduced the likelihood of missing data. We also introduced auto-fill options to minimise typing—an improvement that was especially appreciated by nurses given their workload.
Note: Due to the Service Level Agreement with eFiche, EMR screens cannot be shown.
Tracking data quality
To support SFH, we designed a data-quality tracking approach focused on three initial dimensions:
- Consistency: Comparing self-reported facility footfall with submitted patient files
- Timeliness: Checking whether patient files were submitted on the same day as the consultation and assessing submission patterns across working hours
- Completeness: Verifying whether submitted records included a diagnosis
A weekly dashboard was used to review these metrics, and regular check-ins with health posts were scheduled to gather feedback and identify other issues affecting data quality.
Impact
User testing (pre-deployment)
Before rollout, we conducted user-testing sessions to measure the potential impact of the redesigned interface.
Effectiveness
Using a difficulty scale (Very easy = 1, Easy = 2, Difficult = 3, Very difficult = 4), the new interface consistently scored better across all scenarios. The average difficulty rating improved from 1.89 to 1.22, and all “Difficult” and “Very difficult” ratings were eliminated.
Efficiency
The new interface was faster for two of the three scenarios and slightly slower for one due to a browser-related date-entry issue (since resolved). Overall average completion time improved marginally (12.22 minutes vs. 12.44 minutes).
Preference and satisfaction
All users explicitly preferred the new interface, citing easier navigation, fewer steps, no need to save at every stage, and the benefit of seeing everything on a single page. The Net Promoter Score (NPS) of 33.33 indicated good overall satisfaction.
Data quality outcomes
While multiple interventions contributed to improved data quality (including infrastructure upgrades and digital literacy training), results for the first cohort of digitised health posts were as follows:
December 2024
- Consistency: 51.4%
- Timeliness: 56.8%
- Completeness: 98.2%
November 2025
- Consistency: 99.9%
- Timeliness: 62.9%
- Completeness: 97.3%

Factors such as electricity reliability and internet availability continued to influence results.
Reflections and lessons learned
- Small, well-targeted changes can have outsized UX impact. These improvements should not be underestimated.
- Dashboards need clear and accessible explanations. Metrics must be interpretable to avoid misuse or misinterpretation.
- Digitisation changes how people work, not just what tools they use. Strong onboarding and ongoing support are critical; without them, even good systems risk abandonment.
- It is crucial to account for all external factors that influence a workflow you are designing for - although we do not have influence over RSSB's software or the Ministry of Health's registry, we are able to use our findings to advocate for changes in these processes with both parties, which will be a boon to the health posts.
